It has been almost a year since a state task force finalized recommendations to address Maine’s opioid crisis.
Three separate panels of experts spent months doing research and soliciting ideas. In the end, their recommendations were unanimous. Among them: to immediately expand medication-assisted treatment across the state, to decrease barriers to recovery and to reduce the number of overdose deaths.
But last year, overdose deaths in Maine soared by 40 percent. Gov. Paul LePage is now signaling that when it comes to treatment, he wants the state to try something new.
In his State of the State address Tuesday night, LePage highlighted the latest overdose statistics for Maine: 378 people died from drug overdoses last year. That’s more than one death a day.
For LePage, it’s not only the increasing numbers that are frustrating, it’s the cost of drug treatment that he says is ineffective.
“We’re trying to find programs that work. Because we have so much — we spend over $80 million and it’s not working. Too many people are dying,” he says.
But those on the front lines of drug treatment in Maine say the problem isn’t with existing programs — it’s finding a way to get more people, especially those who lack insurance, into evidence-based treatment such as methadone and Suboxone.
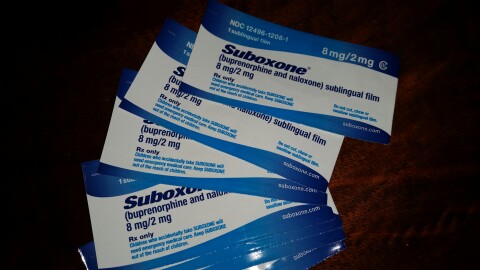
Those medications, in combination with behavioral therapy, have been well studied and are considered the gold standard for drug treatment by the National Institute on Drug Abuse and other health organizations.
In Maine there’s a shortage of it. And the state, advocates say, has done almost nothing to improve the picture.
“We’ve heard story after story after story of people who have spent months and months calling all around the state to try to get help, only to find the same answer,” says Eric Haram, former director of the Addiction Resource Center in Brunswick who now works as a drug treatment consultant.
That answer, Haram says, is often that there’s a wait of at least eight weeks to be seen.
Haram also chaired the state’s treatment task force, convened by the U.S. attorney, the Maine attorney general and the public safety commissioner to address the opioid crisis. He thought the No. 1, unanimous recommendation to expand medication-assisted treatment would be a clear direction to policymakers.
So did Maine Attorney General Janet Mills.
“It’s astonishing to me that a year ago the Legislature authorized and funded ten, only ten, new treatment beds in the Bangor area and yet a year later that hasn’t happened. The beds have not opened. The facility has not opened to a single patient,” she says.
Those ten beds in Bangor are for emergency detox only, not for long-term treatment. And they do not incorporate methadone or Suboxone treatment.
There are private efforts underway to expand the number of Suboxone providers in the state. The state’s ten methadone clinics, meanwhile, are struggling.
“We’ve experienced some recent rule changes that have increased the costs of the services, which creates more of a barrier to treatment,” says Jim Cohen, a spokesman and lobbyist for methadone clinics.
The clinics are currently being reimbursed $60 a week for patients enrolled in MaineCare, a rate that’s been cut by 25 percent in recent years to a level that is believed to be the lowest in the country for methadone treatment. To complicate matters, Cohen says the LePage administration imposed additional counseling and record-keeping requirements and sought to limit patients to two years on the medication, which is often needed for decades.
“Our hope is that the Legislature will revisit this issue, provide the modest amount of funds needed to restore that rate, and allow people in Maine to get the treatment they need,” he says.
Recently, the Maine Department of Health and Human Services set aside $2.4 million to help 350 low-income Mainers access drug treatment. And now Democratic Senate Minority Leader Troy Jackson says lawmakers and the LePage administration are discussing an $8 million proposal to expand medication-assisted treatment to about 700 more people.
Jackson says the proposal combines state and federal funding and was brought forward by DHHS Commissioner Mary Mayhew.
“I think there’s great, great promise, so we’re very interested in going forward with this,” he says.
But right now the proposal is just that. And while the governor signaled in his address Tuesday night that “all options are on the table,” he also said that the state can’t simply throw money at something that isn’t working.